Scarring
Scars occur as a result of injury and normal skin is replaced by fibrous tissue (fibrosis) during the healing process. The difference with a scar and normal skin is the type of collagen that is formed in a scar and the way that it is arranged.
Normal skin shows a strong random network of healthy collagen fibres, whereas in a scar, it is arranged in a single direction and does not contain sweat glands or hair follicles which would be present in healthy skin. Stretch marks (striae) are a particular form of scarring often caused by rapid stretching of the skin as occurs in pregnancy, rapid weight gain or adolescent growth spurts. There are other types of scar where the healing process behaves abnormally resulting in prominent hypertrophic or keloid scars. These can be difficult to treat and may require more specialist treatment.
Early intervention and good wound management is important to prevent the formation of scars and generally the larger the wound and the longer it takes to close, the higher the risk of scar formation. Certain individuals are prone to develop hypertrophic or keloid scarring (dark-skinned people) and this should be taken into account before any invasive procedure. Treating potential causes of scarring such as acne before scarring has developed is important.
The treatment of scars is common practice and generally the younger the scar and the better the skin condition, the more successful the outcome will be. Treatments include collagen induction therapy (Microneedling – Dermaroller and Dermapen) which is ideal for stretch marks and post- surgical scarring, Platelet Rich Plasma and Carboxytherapy can help regenerate the tissue within a scar, Skin peels are good for post-acne scars, Dermal fillers and subcision may be suitable for scars that have sunken below the skin surface, Microdermabrasion will help with superficial scarring and hypertrophic or keloid scarring may require intra-lesional steroid therapy.




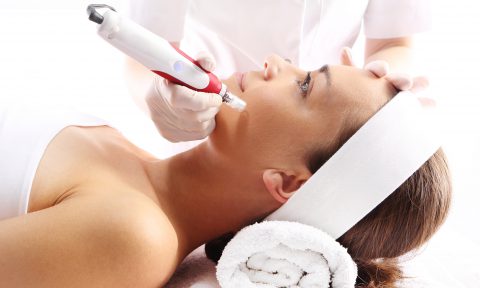


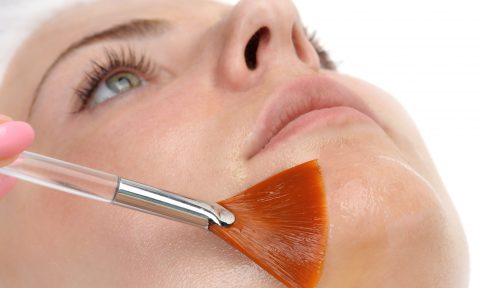










Treatment relies on the body’s healing process so full results not seen straight away, 2 – 3 treatments may be needed, good for general rejuvenation, scars and fine lines.